Patient Eligibility and Verification Services
In today’s healthcare business, Patient Eligibility and Verification Services upfront is the cornerstone of smart Revenue Cycle Management, as it maintains smooth revenue operations. These services confirm coverage, benefits, and payment responsibilities before care begins. By verifying insurance properly, providers cut down on denied claims, get paid faster, and run their practices more efficiently.
Eligibility verification services matter more than ever. Insurance plans are tricky—different costs, different rules. Skip proper checks, and your practice loses revenue, gets late payments, and this frustrates patients. Our eligibility and verification services fix that. We give you clear, up-to-date insurance details when you need them, so you and your patients always know what’s covered.
The Complete Process of Insurance Verification Services
The insurance verification process starts by gathering key patient details—insurance card info, ID, and medical background. Our healthcare insurance verification team double-checks everything through trusted sources to make sure it’s correct and complete.
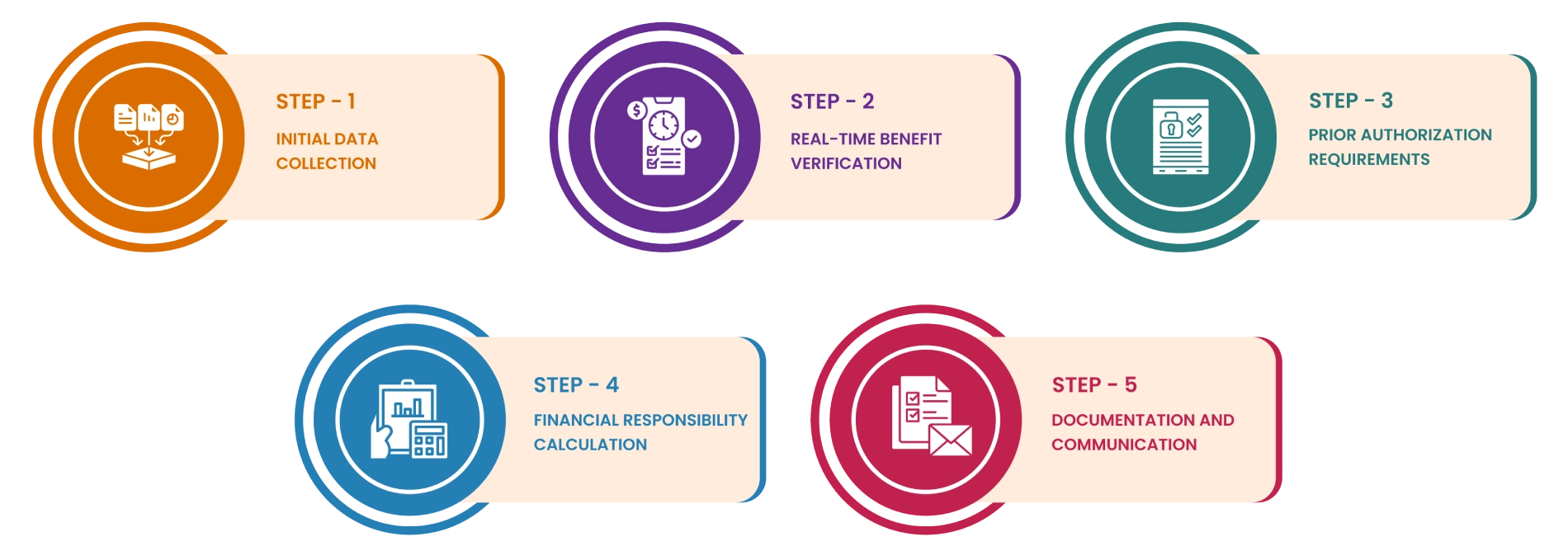
Why Eligibility Verification Matters for Healthcare Revenue Cycle Management
Implementing best practices for checking if someone can get paid for health services (Eligibility Verification Services) is crucial for quick reimbursements and smoother business operations. Practolytics provides top-notch services to help you do this job really well and fast.
Eligibility Verification for 20+ Medical Specialties
Our comprehensive Patient Eligibility and Verification Services make insurance checks easy for doctors. Every specialty is different, so we adjust our services to match. Good insurance verification companies must adapt to deliver providers with effective solutions.
Benefits of Outsourcing Verification to Practolytics
Get in Touch for Seamless Eligibility Verification
FAQs about Eligibility and Benefits Verification
What information is needed to verify a patient's insurance eligibility?
For Patient Coverage Checks, we need: patient name, birth date, insurance card (both sides), Social Security number, policy number, group number, and planned care details. We also ask for the doctor’s NPI number and appointment date. Our fast verification service confirms coverage, benefits, payments due, and approvals needed—so you get paid faster.
How fast can Practolytics verify insurance benefits?
Our insurance verification service gets answers fast: 15-30 minutes for routine checks, 2-4 hours for tricky cases. We also handle urgent requests in 5-10 minutes. Our tech cuts wait times by 60% versus old-school manual checks.
Does your service handle prior authorizations?
Yes—we verify coverage AND handle prior auths start to finish. We spot what’s needed, file paperwork, chase approvals, and update you fast. Works for procedures, specialist visits, scans, and medical equipment orders. No surprises, no delays.
Can this integrate with my existing EHR/EMR?
Our eligibility and verification tools work with major EHR systems like Epic, Cerner, and athenahealth. Setup takes under 2 weeks using secure connections that update in real time.
Can outsourced eligibility verification improve collections?
Yes, Practices collect 25-40% more revenue within 6 months. Our insurance checks cut denials by 35%, speed up payments, and help patients understand costs before treatment—so everyone wins.
Why do 35% of claim denials come from eligibility errors?
Common issues like expired coverage, wrong details, uncovered treatments, missing approvals, and coordination of benefits delays hurt cash flow. Our Patient Eligibility and Verification Services fix these gaps with instant checks and full benefit details—before claims fail.
How does Practolytics verify eligibility 60% faster than manual processes?
We automate data entry, connect directly to payers, use smart tools, and smooth out workflows. Our system spots urgent cases fast while cutting duplicate work—so you get clean claims the first time.
What happens if a patient is found ineligible on the day of service?
Our insurance verification team confirms coverage fast. If there’s an issue, we call patients to discuss options—like self-pay, flexible payments, or a later appointment. Same-day financial help is ready. We also check for backup insurance or urgent approvals when needed.
How much can outsourcing eligibility verification reduce administrative costs?
Organizations typically cut costs by 40-60% by removing staffing, training, and overhead expenses. Our eligibility verification services turn fixed costs into flexible fees, with most practices seeing a full return on investment in just 2-3 months.
Is patient eligibility verification HIPAA-compliant when outsourced?
Yes, our outsourced Medical Insurance Eligibility Verification Services follow strict HIPAA rules. We use BAAs, encrypted transfers, secure storage, and regular checks. Every team member completes yearly training and certification, with security steps that go beyond most clinics’ standards.
Resources
Ensuring a Healthy Workforce: Practolytics’ Expert Medical Credentialing for Occupational Medicine Practices
Practolytics streamlines credentialing for occupational medicine, ensuring compliance, faster onboarding, and a healthier, more productive workforce.
Raising Revenue Efficiency in Vascular Surgery by Using Matching Action’s Medical Billing services
vascular surgery billing with Practolytics. Reduce claim denials, ensure compliance, and improve cash flow with expert RCM solutions.
Streamlining Revenue for Neurosurgery – Medical Billing Services
Neurosurgery billing is complex—Practolytics streamlines coding, claims, and revenue management, reducing denials and administrative burdens for neurosurgeons.